Key facts
- Jaundice turns your skin or eyes yellow. Yellow skin may be less obvious if you have brown or black skin, but you may notice the white part of your eyes looks yellow. Jaundice also makes you feel itchy and causes pale poo and dark urine.
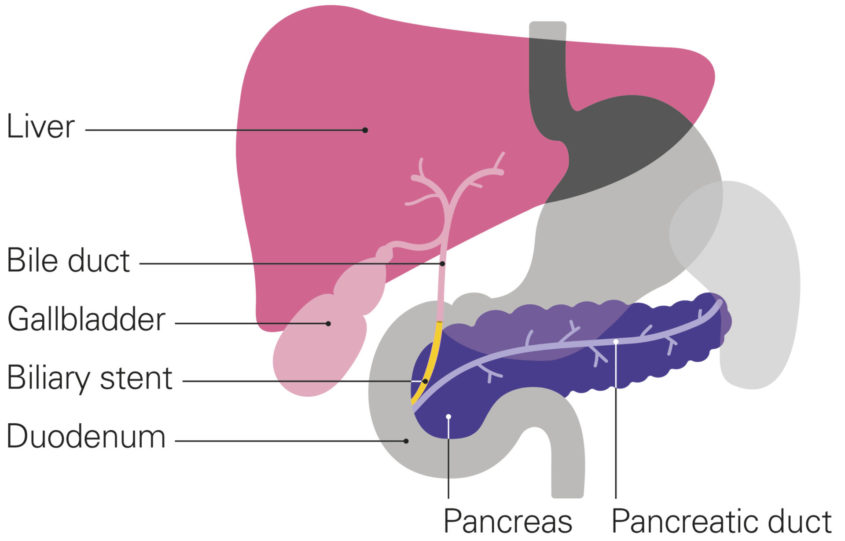
- Jaundice is caused by the cancer blocking the bile duct. Bile is a fluid which helps with digestion. The bile duct is a tube that takes bile from the liver to the small intestine.
- If the cancer has blocked the bile duct, a tube called a stent can be put into the bile duct. This stent is called a biliary stent.
- The stent will open the blockage and treat the jaundice.
- It may take several days for the jaundice to improve and for you to start to feel better.
- Sometimes there can be problems with stents. They can get blocked or move out of place. You could also get an infection or inflammation of the pancreas (pancreatitis). There are ways to manage these problems.
- Talk to your medical team about any questions you have. You can also speak to our specialist nurses on our free Support Line.