Half of pancreatic cancer patients not prescribed tablets they need to stop them starving, new research shows
We launch our new ‘Transform Lives: Prescribe’ campaign, urging the NHS to ensure everyone who could benefit from pancreatic enzyme replacement therapy is prescribed them at the point of diagnosis.
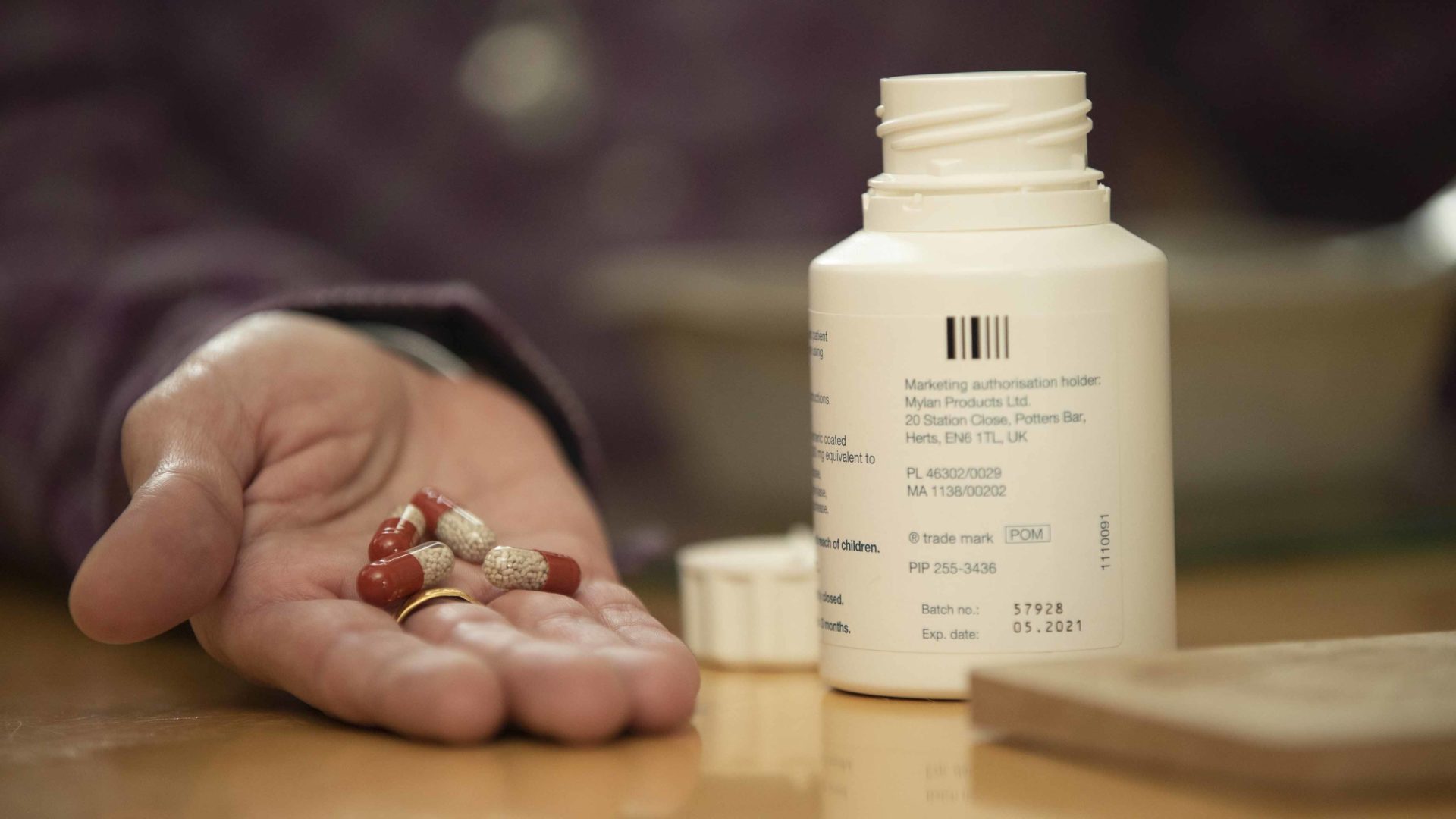
Half of all people diagnosed with pancreatic cancer are not prescribed inexpensive yet essential tablets without which they cannot digest food new research shows – leaving patients less able to tolerate treatment and at risk of starvation. Today (Wednesday 26 May) we launched our new ‘Transform Lives: Prescribe’ campaign, urging the NHS to ensure everyone who could benefit from the tablets are prescribed them at the point of diagnosis.
The alarming finding comes from an audit of 1,350 pancreatic cancer patients in the UK led by researchers at the University of Birmingham, with funding from Pancreatic Cancer UK. The tablets, known as Pancreatic Enzyme Replacement Therapy (PERT), are not new and are already recommended by NICE for people with pancreatic cancer. As the cancer grows it stops the pancreas producing enzymes needed to digest food and absorb nutrients. PERT tablets are therefore essential to help patients eat, stay healthy enough to tolerate treatment and to manage debilitating symptoms from the cancer – including pain, diarrhoea and extreme weight loss.
We are deeply concerned by the low prescription rates, but especially that so many people with incurable pancreatic cancer are not being given the medication – which could not only improve their quality of life, but also help them tolerate life-extending treatment. The audit found that patients who had been diagnosed too late to have surgery (the only potential cure for the disease) are two times less likely to be prescribed PERT tablets. Sadly, 80 per cent of people with pancreatic cancer are diagnosed too late to have surgery. The disease’s vague symptoms, such as back-pain and indigestion, mean it often goes undetected until after it has already spread.
Health professionals’ lack of awareness of PERT tablets is the most significant reason why they are not prescribed more frequently. The majority of the 10,000 people diagnosed with pancreatic cancer in the UK each year are given a terminal diagnosis. They are more likely to be treated by health professionals who do not specialise in the disease and have lower awareness of PERT tablets and their benefits. Cost should not be a factor: at just £7 per patient per day, PERT tablets are inexpensive.
Marie Morris, 44, has seen the devastating impact of the disease. Her mum, Josephine, was diagnosed with pancreatic cancer at a late stage and was never prescribed PERT tablets. Josephine was offered six cycles of chemotherapy to prolong her life but she managed just two before being unable to tolerate anymore. She lost at least two stone in weight from being unable to eat due to the cancer. Frequent vomiting meant she struggled to drink or even swallow painkillers. Josephine died in April 2020 just seven months after diagnosis, aged 73.
Marie said: “It’s hard to see somebody who’s confined to a bed and who can’t eat anything without vomiting. In full health and fitness, she weighed about nine-and-a-half stone. A couple of stone off that… it makes quite a dramatic difference. By the end she was skeletal. There was nothing left, really. Maybe it [PERT] would have made a difference to the length of her life – but perhaps more importantly – also to the quality of her life.”
Through our ‘Transform Lives: Prescribe’ campaign we are urging the NHS across all four nations to implement targets to make sure people with pancreatic cancer are prescribed PERT tablets routinely. Currently more than half of people with pancreatic cancer die within three months of diagnosis. They cannot afford to wait for essential medication and the charity is asking the public to support the campaign by signing its open letter calling for change.
Diana Jupp, CEO of Pancreatic Cancer UK, said:
“Nobody should have to watch someone they love waste away from pancreatic cancer when proven, inexpensive medication is available to stop that from happening. It needs to become second nature to see people with pancreatic cancer and prescribe PERT tablets, in the same way an immediate link is already made between diabetes and insulin. They are just as vital. “Health professionals care for people with pancreatic cancer with great skill and compassion year after year, but many will typically see patients with this devastating disease far less frequently than other types of cancer. People diagnosed with pancreatic cancer cannot wait for the expertise of specialist cancer hospitals to be shared naturally to other parts of the health service.
“We need targeted action now across the NHS to raise awareness of PERT tablets and ensure everyone who needs them is prescribed them – regardless of whether or not their cancer is curable. A simple prescription could give so many people with pancreatic cancer more – and better quality – time with their loved ones.”
Keith Roberts, Pancreatic Subspecialty Lead, Royal College of Surgeons of England said:
“People with heart, lung or kidney failure would not be left untreated, but far too often pancreas failure is. This leads to very predictable problems namely weight loss, abdominal cramps and lack of ability to undergo treatment. Pancreas enzyme replacement therapy is simple and corrects this.”
Mr Richard Wilkin, Clinical Lecturer at the University of Birmingham, said:
“Our important research has highlighted that, despite national guidance, there is a wide variation and under-treatment with Pancreatic Enzyme Replacement Therapy (PERT). This is a very simple tablet that allows patients with pancreatic cancer to absorb their food and is a vitally important part of their treatment. Given that most patients with pancreatic cancer cannot be treated with surgery and are treated in non-surgical hospitals, where prescribing is lowest, strategies to disseminate best practice and overcome barriers to prescribing are urgently required.”
