If it is not possible to remove the cancer, your doctor will talk to you about other treatments, such as chemotherapy. This won’t cure the cancer, but it may help your symptoms and help you live longer.
Speak to your doctor or nurse about whether surgery is an option for you, and whether you will have chemotherapy and radiotherapy.
Getting a second opinion
It can be difficult to tell how close the cancer has grown to blood vessels and whether it is possible to remove it. This means that different medical teams may have different opinions about whether surgery is possible. If your medical team don’t think it’s possible you can ask for a referral for a second opinion from a different team. This may mean going to a different hospital. Be aware that the second team may have the same opinion.
What happens if the surgeon can’t remove the cancer during surgery?
Sometimes the surgeon may start the operation, but find that they can’t remove the cancer. For example, the cancer may have:
- spread to your liver or the lining of your abdomen (tummy area)
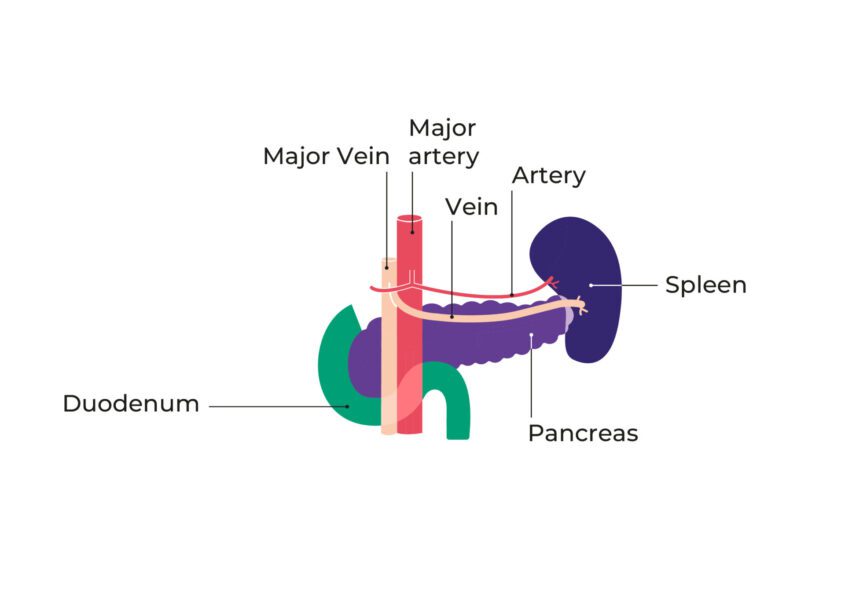
- grown into or around major blood vessels that can’t be removed.
If this happens, the surgeon may switch to a different operation called bypass surgery. This won’t remove or treat the cancer, but it can help with symptoms.
Bypass surgery is still a major operation. Recovery can take at least two to three months. The information about what happens after surgery, side effects and going home after your operation may be helpful.
Finding out that it wasn’t possible to remove the cancer can be upsetting. We are here for you. Read about the support available.