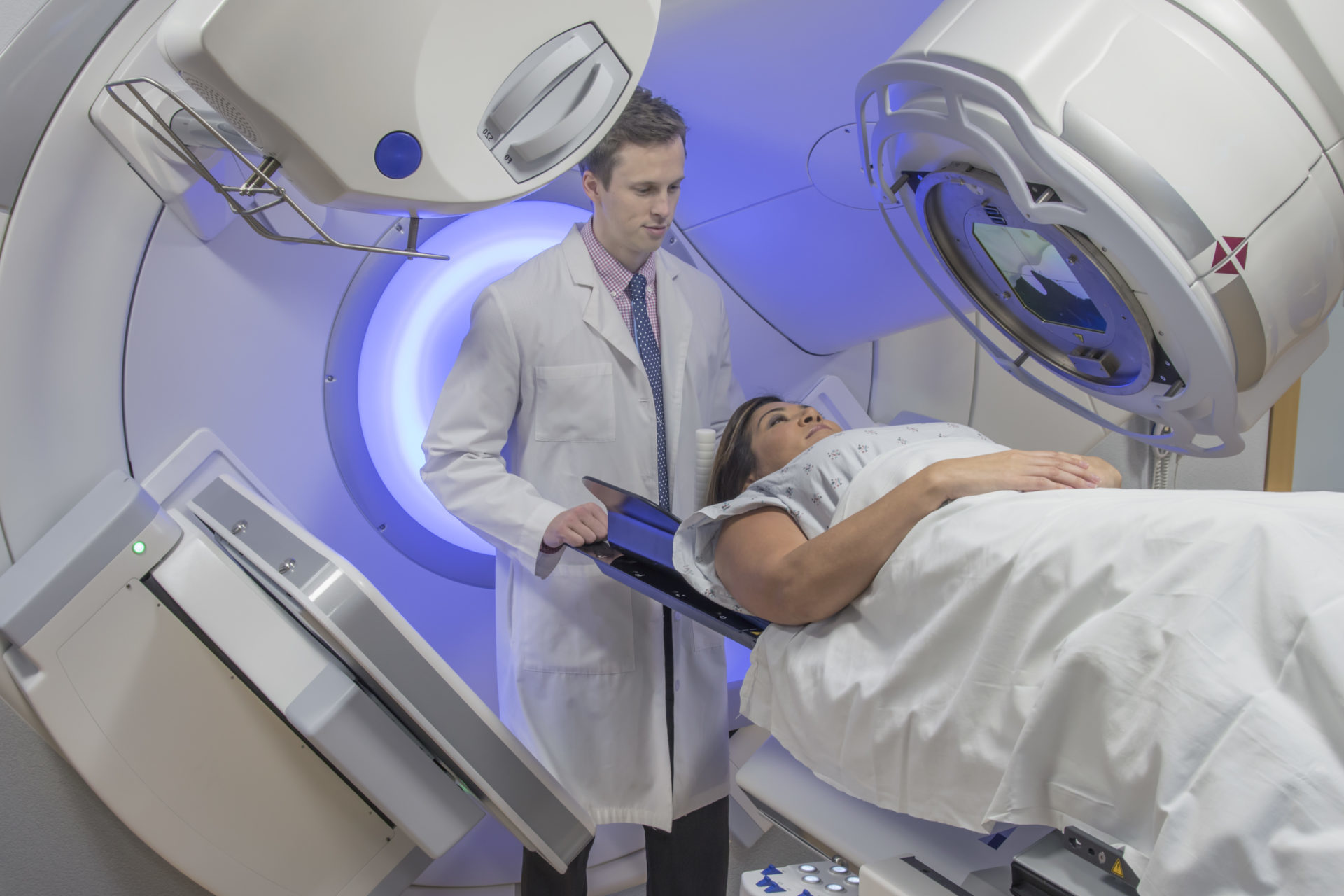
Radiotherapy for locally advanced pancreatic cancer
Locally advanced pancreatic cancer is cancer that has spread to the large blood vessels near the pancreas, or to several lymph nodes.
You may be offered chemotherapy, and then radiotherapy together with chemotherapy (chemoradiotherapy). Stereotactic ablative body radiotherapy (SABR) may also be an option for locally advanced cancer, usually after at least three months of chemotherapy.
Chemoradiotherapy or SABR may help control the cancer and slow down its growth. For a very small number of people with locally advanced cancer, they may shrink the cancer enough for it to be removed with surgery. You will have a CT scan following radiotherapy to see how well it has worked.