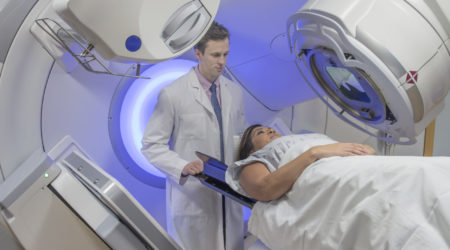
Kate
Kate shares her story of being diagnosed with pancreatic cancer in 2018. She has had FOLFIRINOX chemotherapy and Nanoknife® treatment
I first went to the GP in Feb 2018 as I had been experiencing more heartburn than usual and had pain in my back at night. I was prescribed omeprozole, told I was constipated and to buy some lactulose. I wasn’t worried, I still felt ‘normal’. No weight loss, just a bit more tired than usual, but I put this down to life and age as I was rapidly approaching 60!
Being diagnosed
May came and my heartburn was still troublesome and I had pain under my right ribs. I went back to the doctor who prescribed more omeprozole, a blood test and a CT scan. The following Monday I was called urgently into the surgery and was told I probably had ovarian cancer as my Ca-25 tumour marker levels were raised (Ca19-9 wasn’t checked). A gynaecology appointment was made for the next Monday.
My CT results weren’t back but my GP seemed convinced this was the problem. The following week was spent getting my head around the probable diagnosis and reading about the disease. I was obviously devastated but tried to remain positive as there seemed to be options and treatments available.
After some chasing, my CT results came back and I had another GP appointment to confirm the next steps, only to be told I had pancreatic cancer and not ovarian. Who said it couldn’t be worse… stage IV with multiple liver mets. By this time my Ca19-9 level was off the top of the scale in the many 10,000’s.
Chemotherapy
Then followed a liver biopsy and I started Folfirinox chemotherapy in July, which I was told would give me an extra few months of life if I could tolerate the side effects. Folfirinox can be a brutal regime, but I tolerated it very well.
The first treatment was a shock to the system, especially after a week when I felt absolutely dreadful, tired, stomach cramps, like death warmed up – but this only lasted for a couple of days. As treatment progressed I began to feel better, my pain improved and Ca19-9 levels dropped with each treatment.
I still had side effects, sore mouth, tiredness, tingly fingers and toes, taste changes etc, but tolerable. My hair started to get thinner after four or five sessions, but I didn’t lose it all. I bought a wig in December and wore it for a couple of months, but my hair started to thicken again and I had my shoulder length hair cut short.
Nanoknife® treatment
I wasn’t prepared to sit back and do nothing, so I began to trawl the internet for information about the disease and if there were any other options out there. This was when I first came across an article about Nanoknife® and a lady who had been treated in London who was still alive and well three years later.
Unfortunately, because I have multiple liver mets, I wouldn’t be a candidate for the type of procedure offered here. I joined a Facebook group called ‘Nanoknife Warriors’ and came across a doctor in Miami who performs Nanoknife using an open procedure, and also operates on liver mets. I was impressed with his knowledge about the disease, the articles he has written and the accolades written about him, so sent across my scans and medical records and he agreed to treat me.
I had nine rounds of Folfirinox here which did an amazing job on my tumours and shrunk them considerably, and then I travelled to Florida in January. I had tests and PET scan the day after we arrived and the operation the day after that. All went well. I was in hospital 2 nights and we flew home 2 weeks later. I was well enough to travel down to the Florida Keys for few days at the end of our trip after being given the all clear to travel; although I won’t pretend I felt great!
Having more chemotherapy
I resumed chemo 3 weeks after my operation, and to date have had 12 sessions. My Ca19-9 levels rose a bit initially after the operation, which I was told to expect, but then dropped to 83 – the lowest they have been.
My platelets are unfortunately now taking longer to recover and my neutrophils have been low for the last two, so my chemo sessions have been 4 weeks apart. I have to decide now whether to carry on with chemo as it is, at a reduced rate, or have a break….dilemma!
The next steps
I’m at a bit of a crossroads at the moment. The doctor in Miami likes patients to have SBRT targeted radiotherapy a few months after Nanoknife. I understand this helps break down scar tissue formed by the operation, but my hospital are reluctant to do this. They say it is too risky.
I was thrown another curve ball by my oncologist last Wednesday. Apparently, it has come to light I have been under dosed on one of the chemo drugs way back to my first session. It’s not one of the main components, it’s one that works alongside to aid the chemotherapy’s performance. It should have been administered at a rate of x1.6 according to my height and weight, but I’ve only been receiving the basic x1 dose. No one knows if this has been detrimental, and fortunately I’ve had an excellent response, but I’m very cross this has come to light after 12 sessions.
My oncologist has now agreed to refer me for radiotherapy. I’m not sure what the future holds but I’m not giving up!
May 2019