On this page you will find information about:
Each hospital may do things slightly differently, and treatment will vary depending on your cancer. Speak to your doctor or nurse about your treatment.
Each hospital may do things slightly differently, and treatment will vary depending on your cancer. Speak to your doctor or nurse about your treatment.
FOLFIRINOX is made up of a combination of chemotherapy drugs:
• FOL – folinic acid (leucovorin)
• F – fluorouracil (5FU)
• IRIN – irinotecan
• OX – oxaliplatin.
FOLFOX and FOLFIRI are also combinations of drugs that may be used.
FOLFIRINOX is used in different ways:
FOLFIRINOX is only given to people who are well enough to deal with (tolerate) a few different chemotherapy drugs. This is because it can cause side effects that can be hard to cope with.
Sometimes you may start with a lower dose of some of the FOLFIRINOX drugs to make it easier to cope with. This is known as mFOLFIRINOX (modified FOLFIRINOX). Your chemotherapy team can talk to you about this. Sometimes, if you cope well with it, the dose may gradually be increased.
You will have your chemotherapy at the hospital as an outpatient. This means you will go into hospital for treatment, but you will not need to stay overnight.
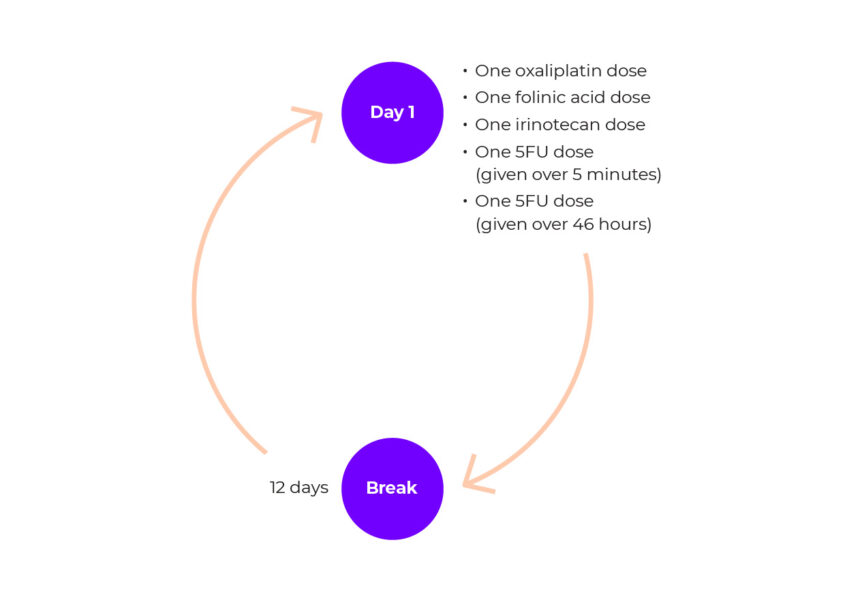
FOLFIRINOX is given in a two week cycle. This means you will have the chemotherapy over two days, and then a break of 12 days before you have the next cycle. The break allows your body to recover. The number of cycles you have will depend on how the treatment is working and how chemotherapy affects you. Your chemotherapy team will talk to you about your treatment cycles.
The FOLFIRINOX drugs are given as an infusion into a vein. You may hear an infusion called a ‘drip’. You will have the infusion through a central line such as a PICC line or a portacath. Read more about central lines, including a diagram of what’s involved.
Each cycle is given in the following way.
Each chemotherapy team may give FOLFIRINOX slightly differently. Speak to your chemotherapy team about how you will be given FOLFIRINOX.
Diagram showing how FOLFIRINOX is given

Some people may have a reaction while FOLFIRINOX is being given. Signs of a reaction are:
These reactions need treating straight away, so if you have any of these symptoms or anything else unusual, tell the nurse who is giving the chemotherapy.
FOLFIRINOX can cause side effects. These can affect everyone differently, and you may not get all the side effects mentioned here. Your chemotherapy team should give you information about any possible side effects and how to manage them. They may give you medicines to take home to help with side effects. Ask the team any questions you have. Knowing what to expect can help you to cope with any side effects.
Your chemotherapy team should give you a 24 hour emergency number to call if you are unwell or have any signs of infection. Or if you need information about any side effects. Your oncology specialist nurse or chemotherapy nurse will explain when to use this number. If you haven’t been given a number, ask them about this.
Fluorouracil (5FU) is broken down in the body by an enzyme called dihydropyrimidine dehydrogenase (DPD). Some people have lower amounts of the DPD enzyme, which is known as DPD-deficiency. People with DPD-deficiency can have side effects that are much worse than usual. These include infections, severe runny poo (diarrhoea) and feeling or being sick.
You will have a blood test to check for DPD-deficiency before you start chemotherapy. If you do have DPD deficiency, you will have 5FU at a lower dose to begin with. If you have not been told about testing for DPD-deficiency, speak to your specialist nurse or chemotherapy team.
FOLFIRINOX can increase your risk of getting an infection. An infection is an emergency if you are having chemotherapy, and needs treating straight away.
Signs of an infection include:
Call the 24 hour emergency number your chemotherapy team will have given you if you have signs of an infection. You should phone if you have any of these symptoms or feel suddenly unwell, even if your temperature is normal or low.
Read more about infections and how they are treated.
If you have diarrhoea, try to drink as much water as you can manage. Call the 24 hour emergency number if you have diarrhoea more than four times a day or are finding it hard to drink enough fluids. You may be given medicines to control the diarrhoea. Your chemotherapy may be delayed until it is better, or the dose of your chemotherapy drugs may be lowered.
Read more about diarrhoea and how it is treated.
Constipation is when you find it harder to poo. Drink as much water as you can manage and try to eat high fibre foods, such as fruit and vegetables. Gentle exercise such as walking can also help. Speak to your doctor about medicines that can help.
Fatigue is a common side effect of FOLFIRINOX. It is not the same as feeling tired. Fatigue can make you feel weak and have problems concentrating.
Some people find that the fatigue starts a few hours to a few days after having chemotherapy and starts to get better a few days later. There are things that you can do to help with fatigue. Read our tips on coping with it .
Oxaliplatin may also cause dizziness. Feeling tired and dizzy can affect your ability to drive. You might want to get someone else to drive you until you know if you are affected.
This is a common side effect of FOLFIRINOX but you will be given anti-sickness medicines to stop you feeling or being sick. If these medicines don’t help, If these don’t help, call the emergency number. You may be able to change to a different medicine. We have tips for coping with feeling and being sick.
FOLFIRINOX can affect the nerves in your hands and feet, which can cause tingling and numbness. This is called peripheral neuropathy. It normally gets better after your treatment finishes. This can be worse in the cold, so wrap up well if you are going outside.
It’s important to tell your chemotherapy team if you have any tingling or numbness in your fingers or toes. They can manage it to make sure it does not become a long term problem. Read more about peripheral neuropathy and how it is managed .
Oxaliplatin can affect your throat, which can make it hard to swallow or breathe. If this happens when you are being given oxaliplatin, tell your chemotherapy nurse straight away. They may stop the infusion of oxaliplatin while they give you medicine to help with this.
You may also get this side effect in the first few hours after having oxaliplatin. This is normally only if you are out in the cold or have a cold drink. It can be scary but is easily treated by having a warm drink. If you are worried, call the 24 hour emergency number you will have been given. This side effect should stop a few days after your treatment finishes. Try to avoid cold drinks and wrap up warm if you go out in the cold.
FOLFIRINOX can lower the number of red blood cells in your blood. This is called anaemia, and can make you feel tired, dizzy or short of breath. If any of these symptoms happen suddenly, call the 24 hour emergency number. If your red blood cell level is very low, you may need to be given blood through a drip. This is called a blood transfusion. Read more about anaemia.
FOLFIRINOX can lower the number of platelets in your blood. This is called thrombocytopenia . You may bruise more easily than normal, and you may be more likely to have nosebleeds or bleeding gums. If you have a nosebleed that does not stop after five minutes, call the 24 hour emergency number.
FOLFIRINOX may cause your hair to thin, or you may lose some hair. But it should grow back once your treatment stops. Read more about hair loss and things that can help.
FOLFIRINOX may cause a funny taste in your mouth. Some people say this tastes like metal or cardboard. You may find that food loses its flavour, or you stop enjoying some foods or drinks. This normally gets better once you finish your chemotherapy. You might find our tips for coping with taste changes helpful.
During your treatment you may not feel like eating, and you may start to lose weight. Try eating small meals often. If your appetite doesn’t get better after a few days, tell your doctor or dietitian. We have tips on dealing with a loss of appetite.
FOLFIRINOX can make your mouth sore, or cause mouth ulcers which can be painful. Tell your chemotherapy team about any mouth problems you have. They can make sure you don’t have a mouth infection and give you a mouthwash which should help. You should also tell them if you have white spots in your mouth. This is a sign of oral thrush, which is normally easy to treat.
FOLFIRINOX can make the palms of your hands and the soles of your feet red and sore. The skin may also start to crack or peel. Your doctor or nurse may give you creams or painkillers to help with this. If you have badly peeling or painful skin, or broken skin that looks infected, call the 24 hour emergency number. The soreness normally gets better when your chemotherapy finishes.
Oxaliplatin can cause problems with your joints, such as swelling or pain. Let your doctor or nurse know if you have this side effect. They can give you painkillers to help. Make sure you check your temperature before taking any paracetamol or ibuprofen. If you have a high temperature, call the 24 hour emergency number straight away.
5FU can make your skin darken or become more sensitive to the sun. Use a high factor sun cream if you are going outside. Tell your chemotherapy team about any skin changes. These changes normally get better when your treatment finishes.
FOLFIRINOX can cause sore, dry, itchy or watery eyes. Tell your doctor or nurse if this happens, as they may need to give you some eye drops. Some people get blurred vision when having FOLFIRINOX, but this is less common.
Fluorouracil (5FU) can cause chest pain. It can also make you feel short of breath, dizzy, or cause an irregular heartbeat. If you have any of these symptoms, call the 24 hour emergency number. If you have chest pain, go straight to A&E and tell them you are having chemotherapy.
Chemotherapy can increase the risk of a blood clot in a vein. If you have any pain or swelling in an arm or leg, or you feel short of breath, call the 24 hour emergency number straight away. Or phone an ambulance and tell them you are having chemotherapy. A blood clot is serious if it’s not treated.
Speak to your chemotherapy team if you have any side effects, or if you would like more information.
You can also speak to our specialist nurses on our free Support Line about FOLFIRINOX and side effects.


You can download our fact sheet on FOLFIRINOX for pancreatic cancer.


Updated May 2024
Review date October 2026